|
Once the embryo reaches the blastocyst stage, an embryologist will take a tiny biopsy of the embryo (cells that will become the placenta) before freezing the embryo. This test checks whether an embryo has the right number of chromosomes (46) or too few or too many.Įmbryos with the complete set of chromosomes are normal, and lead to successful pregnancies and live births, whereas embryos with a chromosomal imbalance are abnormal and fail to implant, lead to miscarriage, or result in an affected baby. Frozen embryo transfer allows for genetic testingįinally, those few weeks on ice before transfer give embryologists time to test the embryo for its chromosomal makeup using Preimplantation Genetic Diagnosis (PGD). Attempting a fresh transfer of this embryo would require placing the embryos in the uterus prior to the time when the embryo is ready or waiting so long for the embryo to get to its optimal stage that the uterus has now lost some of its receptivity.įET permits doctors to freeze the embryo at the blastocyst stage and transfer it at just the right time, when the uterus is most receptive to it, increasing the chances of success. If both embryo and uterus don’t “meet each other” at just the right time, patients miss the chance to become pregnant that cycle.įor example, if a perfectly healthy embryo is growing a bit slowly, it may miss the window of implantation for the uterus. And an embryo can only successfully implant into the uterus once it is mature enough, which is when it reaches the blastocyst stage. The truth is that each cycle, your uterus is only receptive to an embryo for a short window of time, between 24-36 hours. And all this means is that the uterus is ready to receive the embryo, increasing the chances of implantation and ongoing pregnancy. The second benefit of FET, and one that leads to higher success rates, is something we call uterine receptivity. This helps the expectant mother to feel well during the early days of her pregnancy and may reduce the risk of abnormal placentation. With FET, where doctors wait several weeks after egg retrieval to transfer the embryo, a woman’s body has a chance to recover and return to a natural, baseline state. If she were to become pregnant in that time frame, her hormone levels would soar higher, exacerbating her symptoms and placing her at higher risk of ovarian hyperstimulation syndrome, a serious complication of IVF. Potential to reduce the risk of abnormal placentationĪ woman’s hormones are at their highest point right after her eggs are retrieved. Many women note bloating and moodiness during their cycles. While overall safe, in the short term, these medications can make a woman feel, well, hormonal. In order for a woman to grow many eggs during her IVF cycle, she must take ovary-stimulating medications, or hormone injections, for about ten days before her egg retrieval. Let’s dive into each of those benefits, starting with the first. Major Benefits of a frozen embryo transfer & FET Success Rates And the third is that by freezing the embryo, embryologists have time to test it for chromosomal abnormalities prior to transfer.The second is that FET allows doctors to sync up the timing between the embryo and the uterus so implantation can be successful.The first is that FET gives a woman’s body the chance to recover after egg retrieval and before implantation.  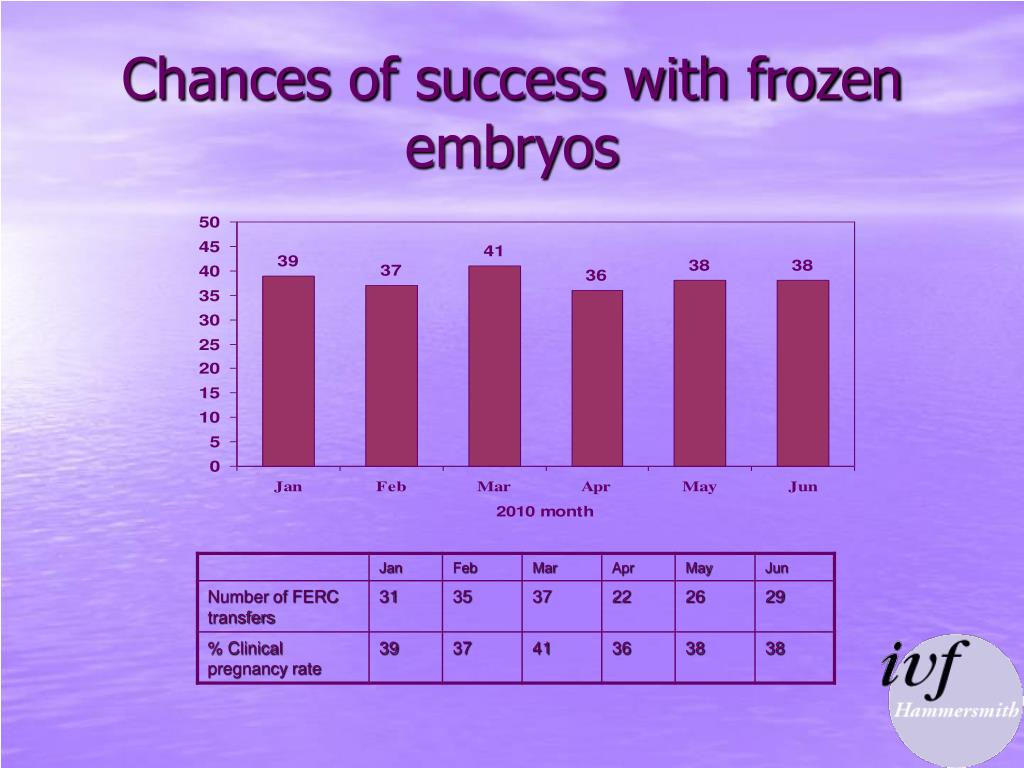
Why frozen embryo transfers? Three reasons: 
Diversity, Equity, Inclusion, and Belonging. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
